A New Generation of Biologically Targeted Radiation Therapy
Combining targeted boron-10 drugs and low-energy neutrons in a novel way to find and treat cancers at the cellular level
Guiding Cancer Treatment from Inside the Body
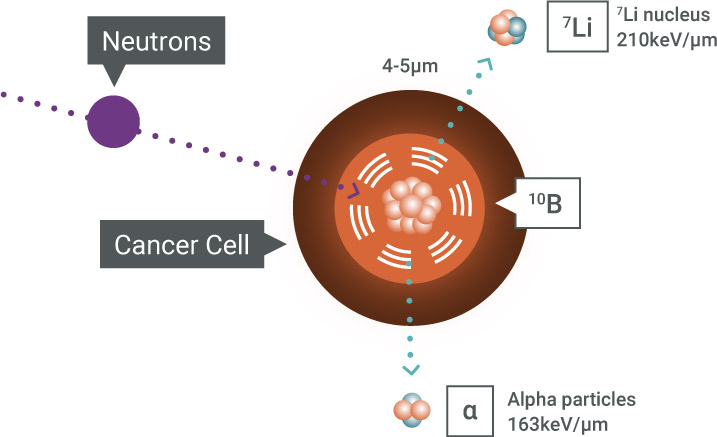
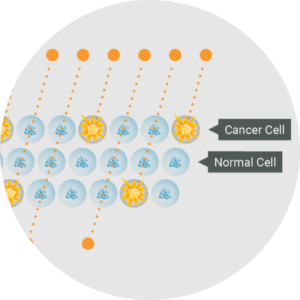
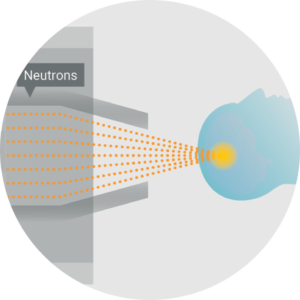
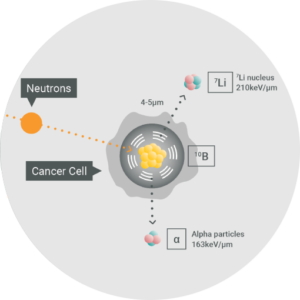
BNCT is an advanced form of radiotherapy that combines the biological targeting precision of a benign boron-10 (10B) target drug with a neutron source to deliver a therapeutic treatment dose only in the cells that contain 10B. The neutrons captured by 10B then generate short-range alpha and lithium particles in the cancer cells that directly create a double DNA strand break in the cancer cells, outperforming other conventional cancer treatments.
BNCT has demonstrated compelling responses for recurrent or refractory cancers, including head and neck cancers, glioblastoma, osteosarcoma, melanoma, liver cancers and has been successful in treating cancer patients for whom other treatment options have been exhausted.
Benefits of BNCT
Cellular-level precision, spares more healthy tissues and can potentially treat cancers that otherwise have few treatment options.
Global research shows BNCT provides the following benefits:
Biophysical Precision

- Effective in treating recurrent, multiple, and untreated cancers
- Targets cancer at cellular level
- Selectively destroys cancer cells
- Eliminates the need for respiratory gating and internal markers
Efficient Treatment

- One to two treatment sessions
- Treats primary and undetected local microscopic cancer cells in parallel
- Potential for more patient throughput than other radiation therapies
Better Patient Experience

- Does not require high-level patient positioning, improving patient comfort and reducing staff workload
- Potential to greatly reduce side effects and improve patient quality of life